At least 374 people in Canada have received a medically assisted death since the practice first became legal in Quebec 10 months ago, The Globe and Mail has found in the most comprehensive survey yet of how often the new end-of-life law is being used across the country.
The vast majority of doctor-hastened deaths – 360, or 96 per cent of the total – happened in four provinces: British Columbia, Alberta, Ontario and Quebec.
Quebec accounted for nearly half of all the assisted deaths The Globe was able to confirm, in part because the province made the option legal six months before Ottawa enacted a law that applied from coast to coast on June 17.
Still, the bare-bones figures that are publicly available do not paint a complete picture of how Canadians, their doctors and their provincial governments are adjusting to a profound change in the way critically ill Canadians can end their lives.
Three provinces declined to divulge any numbers at all, citing privacy, while only two released any details about serious requests that did not proceed, information that could help uncover gaps in access to the fledgling assisted-death regime.
Although the new system is working well in many ways, barriers have cropped up, doctors say.
Some Catholic hospitals are, as promised, transferring out critically ill patients who want assisted deaths; some patients have had trouble finding independent witnesses, leading the advocacy group Dying with Dignity Canada to round up volunteers to sign the paperwork; and some doctors are struggling to balance relieving patients’ pain near the end of their lives with the need to keep them lucid enough to consent at the moment of death.
“We’re hearing that people are afraid to be given medications for pain because it might make them lose capacity,” said James Silvius, Alberta’s lead physician for the new assisted death program. He is looking at developing a guide to help providers with that issue, he said. “The last thing we want is for someone to be in unbearable pain because they’re afraid they’re not going to be able to proceed.”
Jeff Blackmer, the Canadian Medical Association’s vice-president for medical professionalism, said the most common challenge he heard raised at a medical-assistance-in-dying training conference the CMA held in Vancouver last month, was determining who qualifies under a law that says death must be “reasonably foreseeable,” and a patient’s suffering “intolerable.”
“What providers are telling us is a number of them have seen patients who will come and they’ll say, ‘I want an assisted death, but I want it in two months,’” Dr. Blackmer said. “So the physician will say, ‘If you can wait a month or two months, it’s very hard to say that your pain and suffering is currently intolerable.’”
Right now, nobody is tracking these issues at a national level. Health Canada has promised to publish an interim report on medically assisted dying next fall, but the department has not yet decided what information it will collect.
Alberta, which is doing some of the more detailed tracking, has seen 29 completed assisted deaths and 23 cases where a request was not completed, most because the patient either died or lost capacity before two doctors could assess the patients and a 10-day period of reflection had passed.
Quebec’s law, which took effect Dec. 10, required every hospital and hospital network to post their assisted-death statistics up to June 30 online.
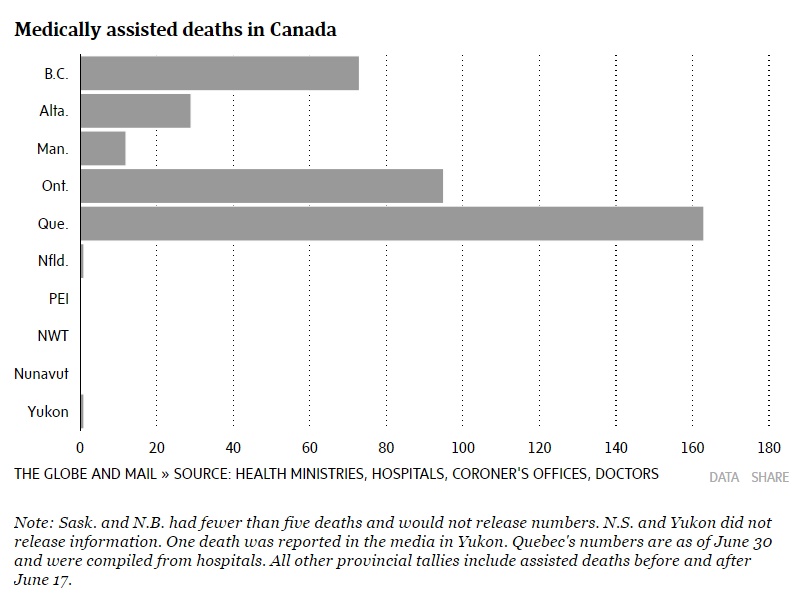
In that time, at least 247 ailing Quebeckers requested a doctor’s help to die, and 163 of them received that assistance, according to The Globe’s compilation.
In Ontario, 95 people have died with the help of a doctor, 13 of them after court orders were granted to patients in the months before the federal law took effect.
Manitoba, meanwhile, reported 12 deaths, and Newfoundland and Labrador reported one. New Brunswick and Saskatchewan would only say there have been fewer than five deaths, citing privacy concerns, and Nova Scotia provided no information for the same reason. Neither Nunavut nor the Northwest Territories have had any assisted deaths so far. Yukon declined to make any information public, but one case has been reported in the media there.
British Columbia’s Coroner’s Office said there have been 66 assisted deaths since June 17. At least seven more were carried out before then by a Vancouver doctor, Ellen Wiebe.
Emilien Gilbert, a Vancouver Island man suffering from congestive heart failure, was among those B.C. patients.
On June 22, five days after medically assisted dying became legal across Canada, the 81-year-old died quietly in the bedroom of his mobile home, guided out of this world by the family doctor who had cared for him for the past 13 years.
Mr. Gilbert was fortunate that his own doctor, Jonathan Reggler, happened to be one of only two physicians in the Comox Valley who had decided to offer medical aid in dying.
Despite preparing thoroughly, Dr. Reggler was nervous. Mr. Gilbert would be the first patient he helped to die.
“I had a week of sleepless nights because I was so anxious about getting it right,” he said.
While Dr. Reggler tossed and turned, Mr. Gilbert’s family prepared to say goodbye. His daughter Suzanne, now 58, flew in from her home northwest of Toronto on Father’s Day, June 19. Brother James, 57, joined them, too.
Youngest daughter, Sandy, 53, who had lived with her father and cared for him since before his wife of 43 years died in 1999, played host to a sort of living wake, with her father’s friends dropping by for a coffee or a beer and a farewell. They reminisced about his childhood in Quebec, his years as a lumberjack and time in the army, the jokes he told in a thick accent that reminded his daughters of former prime minister Jean Chrétien. They bought fresh sheets for the bed where he would die.
“My dad was really calm about the whole thing. He wasn’t shaking. Consequently, nobody had a lot of tears,” Suzanne said. “People were welling up, but I guess everybody was trying to be brave for everybody else. I know I was.”
Suzanne and Sandy stayed at his bedside as Dr. Reggler and his colleague, Tanja Daws, inserted an intravenous line and began delivering the drugs that would end his life.
“The whole experience was peaceful, gentle and just, to me, the way it should be,” Suzanne said.
Dave Miller also found peace in the assisted death of his wife, Storm Miller, even if her good death hasn’t lessened his heartbreak over losing the beautiful and vibrant woman he first fell for at military basic training in Ontario more than 35 years ago.
After the 55-year-old mother of two grown daughters and grandmother of two was diagnosed with incurable stomach cancer – her third new cancer in five years – she sought out help dying. Ms. Miller’s family doctor felt she was not close enough to death and would not help, at least at first.
But once Ms. Miller was referred to Drs. Reggler and Daws, the process sped up and she prepared to die on Aug. 6. Mr. Miller set up a recliner in her beloved sun room and gave her a bouquet of yellow flowers to hug as she died, surrounded by her husband, her daughters, her best friend and her 4-year-old granddaughter.
“It was just a classy way to go: A glass of wine beforehand, saying goodbye to everybody, no trauma,” Mr. Miller said. “Now her loss is what we’re carrying, not the death [itself.]”
KELLY GRANT – HEALTH REPORTER
The Globe and Mail
Published Thursday, Oct. 06, 2016 8:33PM EDT
Last updated Thursday, Oct. 06, 2016 9:40PM EDT